Vitreous and Retinal Detachment
 A common presenting complaint in an eye doctor’s office is the sudden onset of “flashes and floaters”. This generally affects one eye, but can be bilateral. The complaint raises concern about several possible diagnoses, however, posterior vitreous detachment and retinal detachment are most likely. Flashes are typically intermittent and more noticeable in dim light. Floaters may resemble tiny specks, circles, or cob-web like shadows. They will be most notable when looking at a lighted surface, or a white wall. A dilated eye examination is performed to determine the correct diagnosis.
A common presenting complaint in an eye doctor’s office is the sudden onset of “flashes and floaters”. This generally affects one eye, but can be bilateral. The complaint raises concern about several possible diagnoses, however, posterior vitreous detachment and retinal detachment are most likely. Flashes are typically intermittent and more noticeable in dim light. Floaters may resemble tiny specks, circles, or cob-web like shadows. They will be most notable when looking at a lighted surface, or a white wall. A dilated eye examination is performed to determine the correct diagnosis.
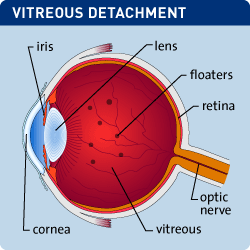
The vitreous body is a clear gel-like structure that fills the space between the lens and the retina. It is weakly attached to the retina at several points along retinal blood vessels and at the optic nerve head in the back of the eye. It is more firmly attached to the wall of the eye anterior to the retina. As people age, the vitreous liquefies and the posterior attachments break down. This results in the acute change referred to as a posterior vitreous detachment (PVD). A PVD is frequently associated with complaints of seeing flashes and floaters. The flashes tend to stop within a few days when the detachment is complete. Observation of floaters may persist considerably longer, however, after a few months many patients report that they infrequently notice floaters with some not seeing them at all. PVD is a normal condition associated with aging and does not require any treatment. Observation for signs and symptoms of retinal detachment is recommended for a six week period following the onset of symptoms.
The retina is the neural tissue the lines the inside of the wall of the eye posterior to the lens. Retinal detachment is a condition defined by separation of the thin retinal tissue layer from the layer of blood vessels beneath it that provides oxygen and nourishment. The longer a detachment goes untreated, the greater your risk of permanent vision loss in the affected eye. Symptoms of a retinal detachment include the sudden appearance of flashes and floaters, blurred vision, gradually reduced peripheral vision, and a curtain-like shadow over your vision.
The most common type of retinal detachment is referred to as a rhegmatogenous retinal detachment. This results from a hole or tear in the retina that allows fluid to collect underneath the retina. The most common cause of rhegmatogenous retinal detachment is aging and the development of a PVD. A PVD may be complicated by development of a retinal tear and detachment. People with high myopia (extreme nearsightedness) are more likely to develop a retinal detachment associated with PVD. Tractional retinal detachment develops when scar tissue grows on the retina’s surface. This type of scar tissue is typically seen in patients with poorly controlled diabetic retinopathy and other conditions. Exudative retinal detachment can be caused by age related macular degeneration, injury to the eye, ocular tumors, and inflammatory disorders.
Retinal detachment is treatable in a variety of ways. First, it is important to ascertain the reason the retina is detached. This can often be accomplished with a dilated eye examination. If the interior of the eye cannot be observed due to bleeding, an ultrasound examination of the eye can be helpful. If a rhegmatogenous retinal detachment is diagnosed, then a variety of microsurgical techniques can be used to push the retina back into place and seal any tears or holes. Tractional retinal detachment requires release of the retina from scar tissue that can be accomplished with microsurgical intervention. Exudative retinal detachment is addressed by treating the underlying pathological process, either with medication, laser, intraocular surgery, or some combination of these methods.





